
Patients were placed in a prone position on the CT table and imaging was completed though the level of the pars defects. Staff experience ranged from 2 years to 25 years with an average of approximately 10 years of staff experience in CT-guided procedures. Board-certified, fellowship-trained neuroradiologists and musculoskeletal radiologists trained in CT-guided spine interventions completed all injections. Preprocedure informed consent was obtained from all patients. Resources were limited for this database and, therefore, our ability to complete extended follow–up was accordingly limited. At least three attempts were made to contact each patient at each time point. An independent paramedical assessor obtained follow-up R–M and NRS data via telephone call at 2 weeks and 2 months post procedure. All patient data were entered into an SAS database (SAS Institute, Cary, NC, USA). Immediately prior to the procedure, patients completed two outcome measures: the Roland–Morris disability questionnaire (R–M, 24 questions) and a pain numerical rating scale score (NRS, 0–10, in which 0 was no pain and 10 the worst pain imaginable). If a patient received multiple pars injections separated by more than 2 months, outcome data related to the first injection were considered for this study. Patients who received multiple pars defect injections or other co-interventions, including injections directed to other potential pain generators, within 2 months, were excluded. The diagnosis of pars defect was made on preprocedure cross-sectional imaging, typically CT exam. The study cohort included 59 patients undergoing a single segmental level CT-guided pars defect injection from 2006 to 2012. The study was approved by the local Institutional Review Board and complied with all Health Insurance Portability and Accountability Act requirements. (C) Terminal stage: wide defect with rounded margins and sclerosis. (B) Progressive stage: fissure that was still narrow but had slightly rounded margins. (A) Early stage: narrow fissure through the pars with sharp margins. 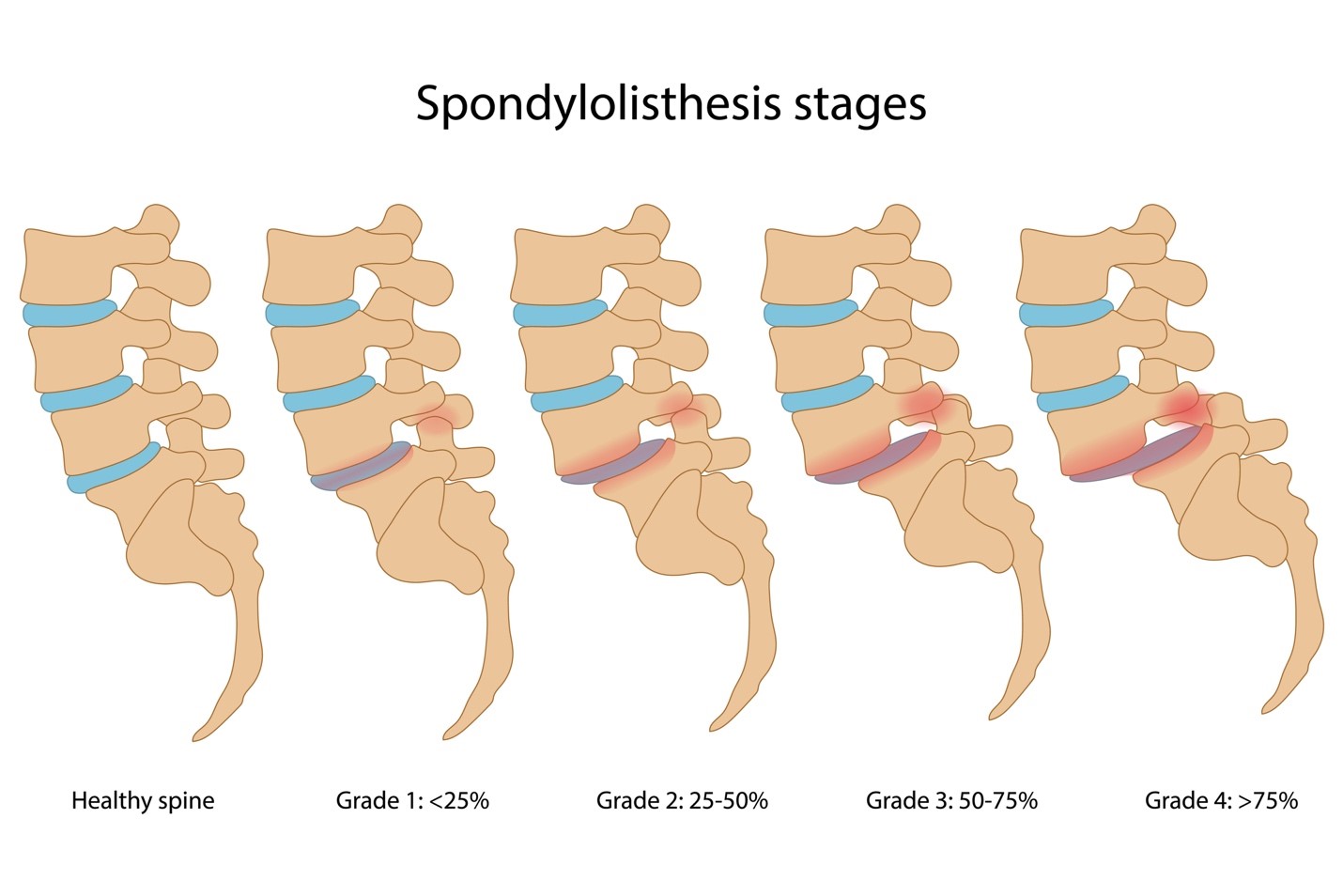
Pars interarticularis fracture stages (dashed circles). CT guidance allows placement of a needle directly into the bony spondylolytic defect and distribution of pharmaceuticals into the surrounding fibrocartilaginous mass, as well as exclusion of injectate migration into the epidural space. Inflammatory enhancement in this fibrocartilaginous mass at the lytic defect may be seen on MR imaging. On CT imaging, terminal lesions have smooth sclerotic margins and are accompanied by a fibrocartilaginous mass in up to 90% of cases. Terminal lesions have no healing potential and are the lesions under consideration as axial pain generators in this study. 
The early and progressive lesions have healing potential with bracing and conservative measures and are typically seen in adolescent athletes. Fujii and colleagues categorized these as early, progressive and terminal changes (Figure 0001). Spondylolysis is extremely rare in the infant population but appears to develop in childhood or adolescence, with no significant change in its incidence beyond age 20.Ĭomputed tomography (CT) allows characterization of the structural change in the pars as a stress response (sclerosis), an incomplete fracture, or a completed fracture. It occurs most commonly at the L5 level (67%), followed by L4 level (15–20%), and 元 (1–2%). Spondylolysis has a familial predisposition there is a 2–4:1 male-to-female predominance. Spondylolysis is considered a fatigue fracture occurring within a vulnerable pars the vulnerability may be related to the distribution of ossification centers within the posterior neural arch, not a deficit in bone quality. However, the vast majority of these patients are asymptomatic. Pars defects, also termed spondylolysis, are relatively common, with a prevalence of 7% in the U.S. In patients with axial low pain who harbor chronic pars interarticularis defects, this lesion may also represent a pain generator. In patients with axial low back pain, the primary pain generators considered to be amenable to percutaneous diagnosis or therapy are the intervertebral disc, the sacroiliac joint, and the zygapophyseal joint. Corticosteroid, CT, Injection, Pain, Pars Interarticularis Introduction
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
